Stop leaving revenue on the table
The average primary care practice undercodes by 10–15%. Medicare beneficiaries see seven providers a year, but your EHR only knows what happens in your four walls. Sguardo pulls every record together, normalizes it to a research-grade standard, and gives you the analytics to recover missed HCC codes, close care gaps, and negotiate payer contracts from a position of data.
Runs on your infrastructure (on-prem or cloud). HIPAA audit trails built in. Your data never leaves your control.
Sguardo is currently in limited private beta. Request an invite and we'll get you set up personally.
Request Limited Private Beta Invite Learn More
Why practices stay stuck
You can't improve what you can't measure , and right now, most practices can't measure much at all.
Your EHR sees one room
Claims data arrives weeks late. External records come by fax. A typical Medicare beneficiary sees seven providers a year , and you're making clinical and financial decisions with a fraction of the picture. Sguardo aggregates what every other system misses.
Quality reporting is a scramble
When your data lives in silos with inconsistent coding (SNOMED in one system, ICD-10 in another, free text in a third), computing accurate HEDIS scores or identifying care gaps requires heroic manual effort every reporting season. Sguardo runs those computations continuously, not annually.
Missed codes cost real money
Undercoding costs the average primary care practice 10–15% of potential revenue. HCC codes get missed because they require complete clinical context (which no single system has). Contracted rates drift below market without anyone noticing. Without data, you negotiate blind.
For fee-for-service practices
You don't need to be in a VBC contract to benefit from Sguardo. Most practices leave money on the table in FFS. We help you find it.
Understand your practice economics
Sguardo breaks down your revenue by procedure, payer, and provider, showing you exactly where your FFS income comes from. See which services are profitable, which payers reimburse below market, and where coding improvements would increase revenue without changing how you practice.
Identify underpaid services
Compare your contracted rates against the Medicare Physician Fee Schedule and regional commercial benchmarks. Sguardo flags specific CPT codes where your reimbursement is below the 25th percentile , and generates the supporting data you need to request a rate increase at your next payer contract renewal.
Optimize coding accuracy
Undercoding costs real money. Sguardo analyzes your claims history to identify patterns of consistent downcoding: procedures billed at lower complexity than clinical documentation supports , and gives your coders specific, actionable feedback.
Benchmark against peers
Compare your reimbursement rates against regional and national benchmarks using CMS fee schedules and publicly available transparency data. Know where you stand , and where renegotiation will have the highest revenue impact.
Your pathway from FFS to value-based care
The transition doesn't have to be all-or-nothing. Sguardo helps you move at your pace, starting with low-risk steps that improve your FFS practice and building toward full VBC readiness.
Optimize FFS
Start by understanding your current economics. Fix undercoding, identify underpaid services, and negotiate better rates. This generates immediate revenue (no contract changes needed.
Enroll in CMS DPC
DPC gives you Medicare claims data for your attributed patients, the foundation for population health analytics. Sound Prediction helps with enrollment and handles the technical integration.
Build quality metrics
With DPC data flowing, Sguardo computes your HEDIS scores, identifies care gaps, and tracks HCC coding accuracy. You'll have 6-12 months of quality data before signing any VBC contract.
Enter VBC with confidence
Model contract terms against your actual panel data. Know your projected savings before you sign. Sguardo continues to track performance, flag risks, and generate the reports you need for payer negotiations and renewals.
For value-based care practices
With clean, normalized data in place, Sguardo delivers the analytics that drive VBC performance.
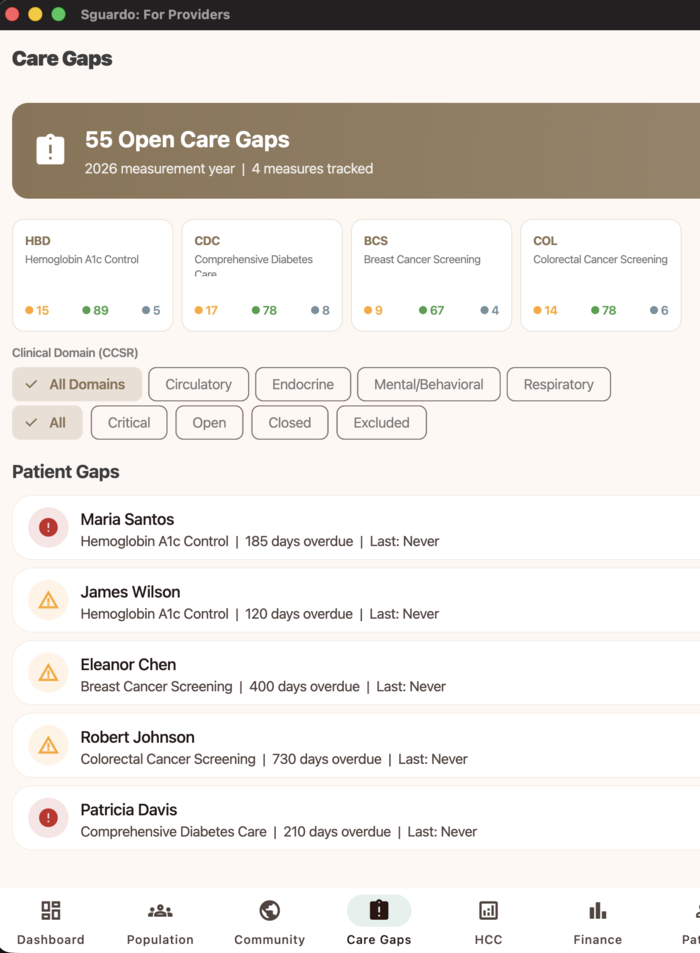
Care Gap Identification
Sguardo identifies patients who are due or overdue for evidence-based interventions across HEDIS measures: HbA1c testing and control, blood pressure control, statin therapy for cardiovascular disease, and cancer screenings. Each gap surfaces as an actionable item with patient context and clinical rationale.
HCC Risk Adjustment Coding
Sguardo identifies Hierarchical Condition Category codes from your clinical and claims data, surfacing coding opportunities that reflect true patient acuity. Accurate HCC coding directly impacts risk-adjusted capitation payments and ensures your patient population's severity is properly represented.
Population Health Dashboard
View your patient panel stratified by risk level, chronic conditions, and care gaps. See where to focus resources: which patients need outreach, which cohorts are trending poorly, and where your quality scores stand.
Total Cost of Care (TCOC)
Track your attributed population's total cost of care with IBNR adjustments for claims lag. Identify high-cost patients and rising-risk cohorts, project shared savings before reconciliation, and get early warning alerts when you're trending above target spend.
Quality Measures
Sguardo computes eCQMs and HEDIS measures directly from OMOP CDM data. Numerator/denominator logic runs on normalized, deduplicated records rather than whatever your EHR happens to capture. More accurate measurement, fewer surprises at reporting time.
Reference Range Evaluation
Every lab result is automatically evaluated against 500+ reference ranges, stratified by age, sex, fasting status, pregnancy, and specimen type. Your team sees which values are borderline and which are critical, in context for each patient's clinical profile.
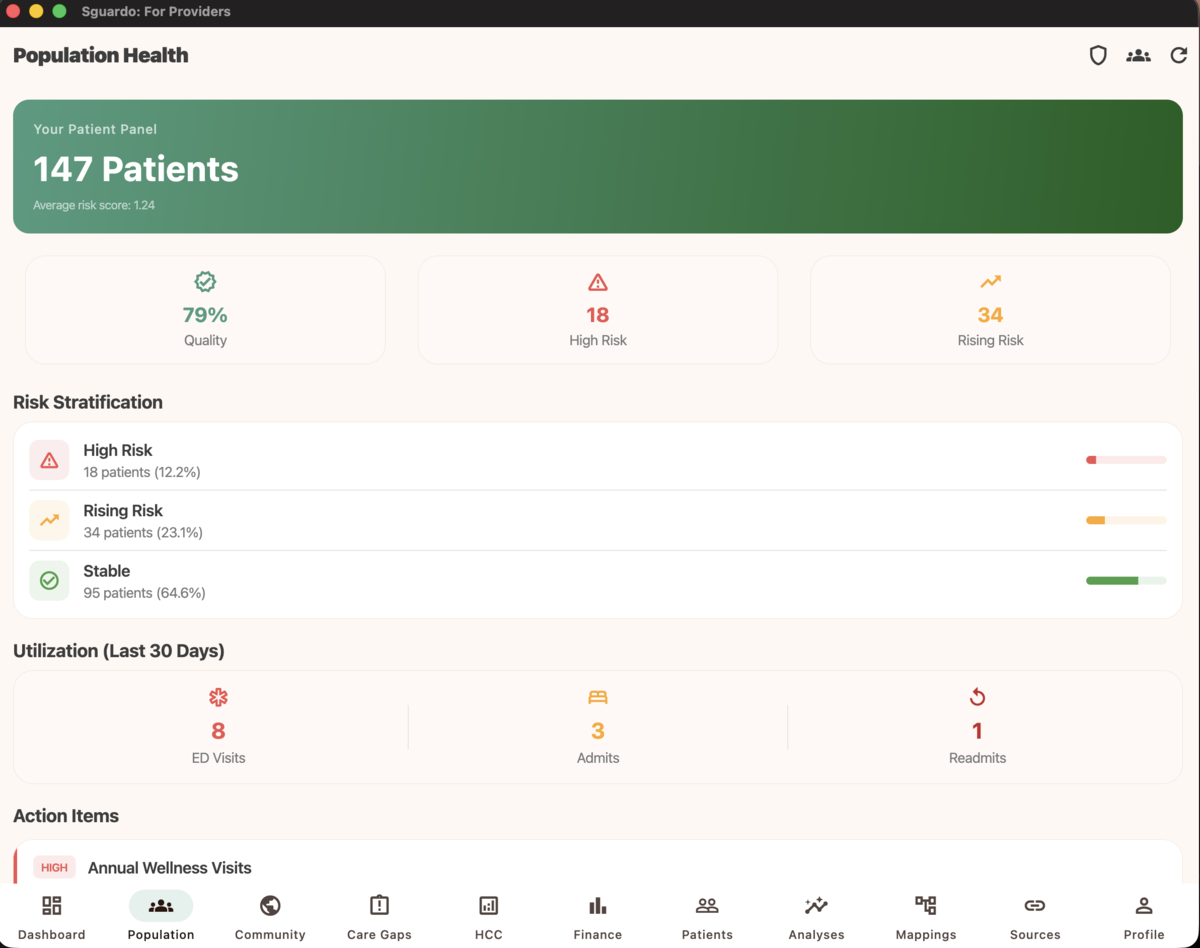
Population Health — Risk stratification, utilization metrics, and action items at a glance
Data infrastructure
Every feature in Sguardo depends on the same thing: clean, normalized, complete data. Here's how we produce it.
SMART on FHIR EHR Integration
Sguardo supports EHR-initiated SMART on FHIR launch: clinicians open Sguardo directly from Epic, Cerner, or any SMART-compliant EHR without a separate login. FHIR R4 resources (Patient, Observation, Condition, MedicationRequest, Procedure) sync into OMOP CDM in the background.
CMS DPC & Blue Button
Sguardo manages the entire DPC lifecycle: organization registration, practitioner attribution, patient roster sync, and automatic conversion of claims into OMOP CDM records. Blue Button 2.0 roster management tracks authorization status across your Medicare panel with proactive re-consent alerts. Sound Prediction helps practices onboard into the CMS DPC program.
OMOP CDM Standardization
Every data source (EHR exports, claims feeds, legacy databases, FHIR bundles) is normalized to the OMOP Common Data Model. Full Athena vocabulary integration: SNOMED CT, RxNorm, LOINC, ICD-10, HCPCS, and CPT. CDM versions 4.0 through 6.0, including Oncology extensions.
Schema Discovery
Sguardo's schema discovery engine (inspired by OHDSI's WhiteRabbit methodology) connects to any source (PostgreSQL, MySQL, SQL Server, Oracle, CSV, Parquet) and inventories every table and column, profiles value distributions, and measures completeness. The scan runs without extracting PHI, safe for production databases.
Visual ETL Mapping
Drag source tables to OMOP CDM targets in a visual editor. Sguardo auto-generates field mappings with confidence scores using deterministic concept matching and stem table architecture. The output is executable DuckDB SQL, reproducible and auditable.
DuckDB Analytics Engine
Vocabulary queries and analytics run on DuckDB (no separate import step, no heavyweight database. 2.4 million OMOP concepts queryable in milliseconds. Vocabulary-aware SQL generation resolves source codes to standard concepts automatically.
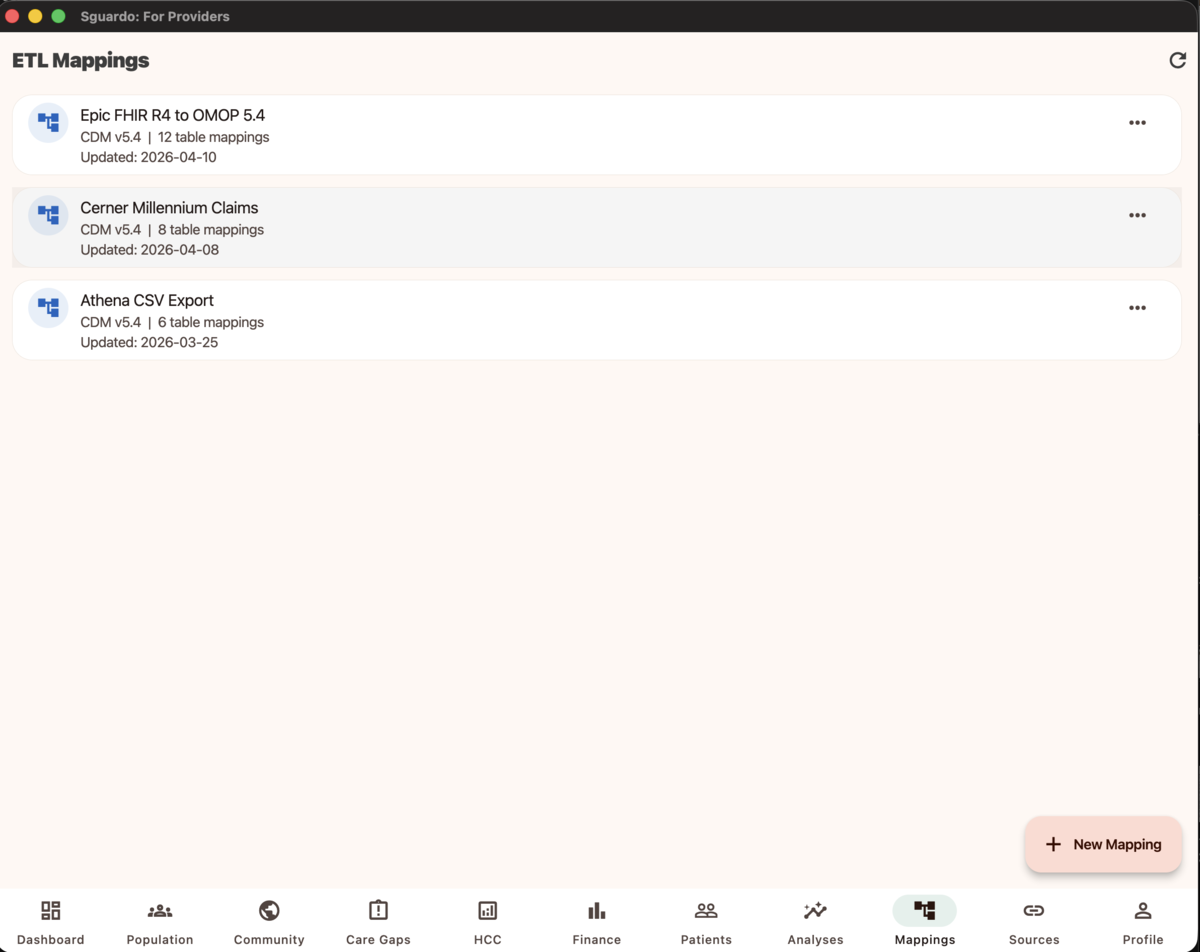
ETL Mappings — Epic FHIR, Cerner, Athena and more mapped to OMOP CDM
Financial decision support
Whether you're in fee-for-service, transitioning, or already in a VBC contract, Sguardo gives you the data to optimize revenue and negotiate from strength.
Payer Negotiation Reports
Generate data-backed negotiation packages ready to present to payers. Sguardo compiles your quality metrics, cost savings, patient outcomes, and benchmark comparisons into structured reports, giving you leverage whether you're negotiating FFS rates, shared savings terms, or capitation arrangements.
Reimbursement Benchmarking
Compare your reimbursement rates against regional and national benchmarks using CMS fee schedules and publicly available transparency data. Surface where you're being underpaid and identify the specific CPT codes and payers where renegotiation will have the highest revenue impact.
VBC Contract Modeling
Model the financial impact of value-based care contracts before you sign them. Project revenue under different shared savings arrangements, capitation rates, and quality bonus structures using your actual patient panel data and historical utilization patterns.
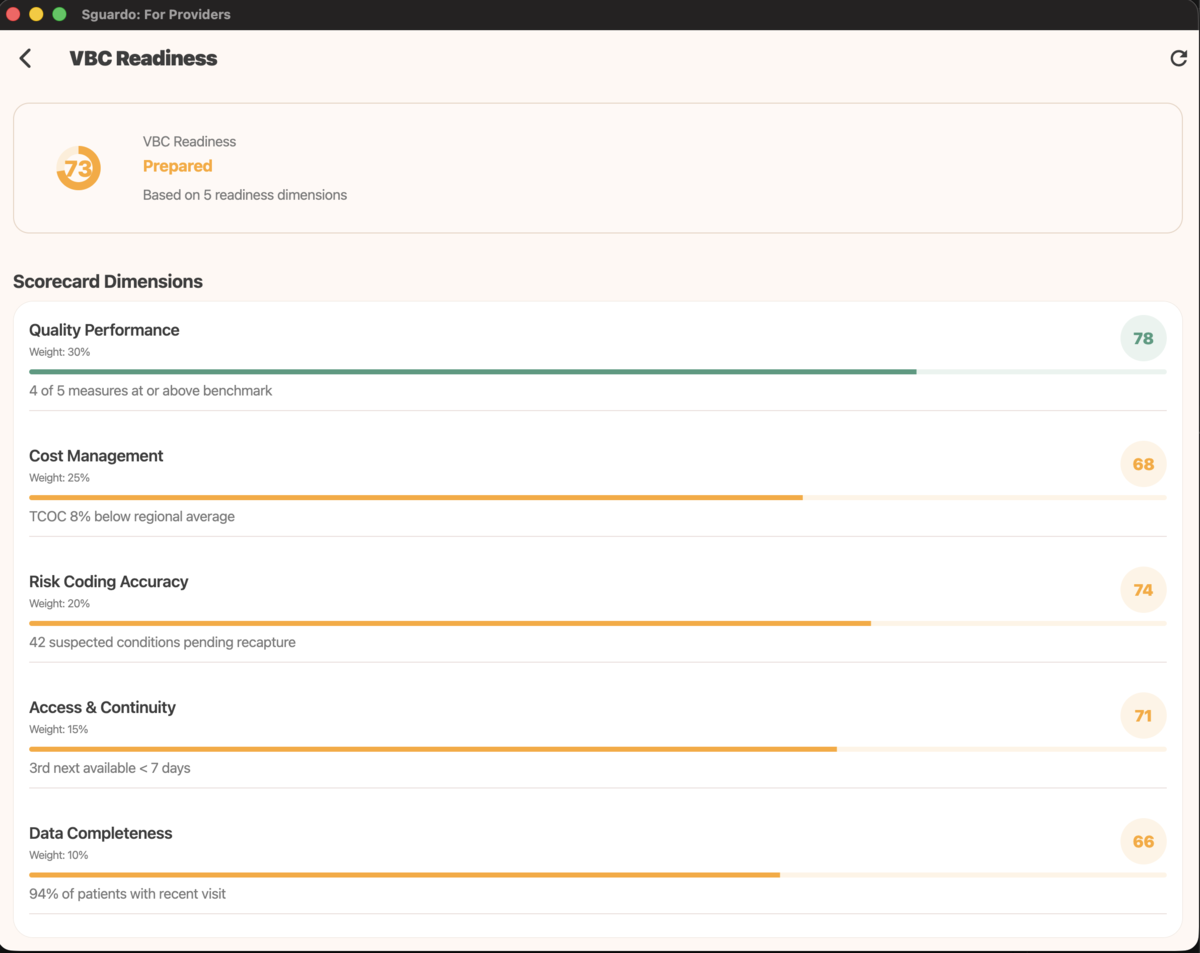
VBC Readiness — Quality, cost, risk coding, access, and data completeness scores
Why not just use your EHR's built-in tools?
Typical EHR Analytics
- Siloed to data entered within that single EHR
- Missing claims history and external encounters
- Limited vocabulary mapping across coding systems
- Vendor-proprietary data formats
- Analytics modules at additional licensing cost
- No financial modeling or payer negotiation tools
- Cloud-only . Your data on someone else's servers
Sguardo
- Aggregates data from all connected sources into OMOP CDM
- Full CMS claims + clinical data picture per patient
- Automated terminology normalization (ICD, SNOMED, RxNorm, LOINC)
- Open standards from the ground up: FHIR R4, US Core, USCDI
- Quality measures, HCC coding, care gaps, and population health included
- FFS rate analysis, VBC contract modeling, reimbursement benchmarking
- On-prem or private cloud: data stays under your control with HIPAA audit trails
Security and compliance, built in
On-Prem or Cloud
Sguardo deploys within your own infrastructure — on-prem behind your firewall or in your own cloud tenant. No data leaves your environment.
HIPAA Audit Trails
Every PHI access is logged with structured metadata. Request bodies are deliberately excluded to prevent PHI from appearing in logs.
Zero-Trust Auth
OAuth2 with PKCE, HTTP-only SameSite=Strict cookies, CSRF protection, and role-based access control. SMART on FHIR launch context for EHR integration.
Encrypted at Rest
Credentials encrypted in storage. OAuth tokens with automatic expiration. TLS enforced for all connections.
Visual ETL mapping (no code required
Drag source tables to OMOP CDM targets. Sguardo auto-generates field mappings with confidence scores, then produces executable DuckDB SQL.
Source Tables
Active Mappings
OMOP CDM 5.4
Sguardo ETL Mapping Interface — Rabbit-in-a-Hat style visual mapping from source schema to OMOP CDM
Ready to see the full picture?
Sguardo is in limited private beta. Request an invite and we'll walk through it with your actual workflows — care gaps, HCC coding, financial benchmarks, or OMOP ETL setup. Bring your hardest data problems.
Request Limited Private Beta InviteOr email us directly at info@mederrata.com — we respond within one business day.



